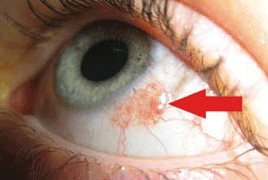
INTRODUCTION: The etiology of papilloma formation is multifactorial. There is a strong association between human papillomavirus (HPV) and the development of these conjunctival lesions. HPV is tumorigenic and commonly produces benign tumors with low malignant potential. Papillomas rarely go through malignant transformation.
MATERIAL AND METHODS: Retrospective study of patients with a diagnosis of conjunctival papilloma or squamous cell carcinoma.
RESULTS: In a collection of 125 patients in the period 2007–2017, 119 (95.2%) were confirmed by papilloma histological examination in 119 (95.2%) and in 6 (4.8%) patients with carcinoma. Of the total number of patients, 39 were women (31.2%) and 86 men (68.8%). The mean age of patients was 68.4 years (range 20–94 years). Localization of lesions: bulbar conjunctiva 65 (52.0%), upper eyelid tarsal conjunctiva + fornix 6 (4.8%), lower eyelid + fornix 27 (21.6%), caruncle 20 (16.0%) and plica semilunaris 7 (5.6%) patients. In the patient population we recorded 2 papillomas that were transformed into squamous cell carcinoma. HPV16 was positive in these patients, the carcinomas were from the area of the bulbar conjunctiva, and the surgical solution was associated with the perioperative administration of Mitomycin C. In one case, the inverted papilloma developed into orbital carcinoma within 2 years of primary excitement, and the patient underwent radical surgical procedure (partial exenteration of the orbit) followed by radiotherapy.
CONCLUSION: Transformation of the papilloma into the carcinoma is rare, but it must always be thought of as a recurrence of the disease. HPV can infect the conjunctiva. The ophthalmologist, in collaboration with a pathologist, may recommend appropriate laboratory tests to confirm the diagnosis. Outpatient follow-up of patients after excision of the joint papilloma is also necessary.