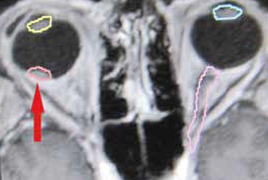
Introduction: Nowadays radiotherapy is the standard treatment care for patients with uveal melanoma. In Slovakia the only one option is a one-day session stereotactic radiosurgery at linear accelerator LINAC. Irradiation of surrounding tissues of the eye and orbit causes radiation complications. One of the most serious and vision-threatening is the radiation retinopathy, which divides into maculopathy and peripheric retinopathy. The clinical signs include microanerysms, teleangiectases, hard exsudates, cotton wool spots and macular edema, neovascularisation, and vitreous hemorrhage. Radiation macular edema can be classified by optical coherence tomography into cystoid or noncystoid edema. On fluorescein angiography macular edema is divided into non-ischemic and ischemic, while the latter means usually irreversible loss of the visual acuity. This paper is focused on risk factors of radiation retinopathy although it strongly influences functional result of radiotherapy and preservation of the visual acuity.
Purpose: By means of bivariate and multivariate analysis to determine the association of radiation dose and other variables with the development of radiation maculopathy.
Material and methods: The retrospective analysis of 168 patients with ciliary body or choroidal melanoma who performed one-day session stereotactic radiosurgery on a linear accelerator LINAC in a period 2007–2016.
Results: The prevalence of the radiation maculopathy was 29% with the median time from the irradiation to maculopathy 16 months. Median radiation dose on the macula was 37 Gy. Variables statistically significantly associated with the maculopathy were: radiation dose (p = 0.0016), postequatorial location of the tumor (p = 0.0271) and better visual acuity before treatment (p = 0.0007). The tumor touch of the macula was strongly associated with the visual acuity in the bivariate analysis (p = 0.0006), thus it could be omitted from the final model. Discussion: The radiation dose on a macula is the key determinant for radiation-induced maculopathy, according to other authors and our study approvingly. Other variables were related to proximity of the tumor to the macula, so the radiation dose on the macula was higher indirectly. Better visual acuity before
treatment as a risk factor for maculopathy can be a consequence of: a) earlier diagnostics of tumor with proximity to the posterior pole, b) lower enucleation rate; frequency of the enucleation was 1.6 higher in patients without maculopathy. Naturally, on enucleated eyes maculopathy was not diagnosed. Five patients underwent intravitreal application of the bevacizumab as a treatment of the radiation maculopathy, without improvement of the visual acuity.
Conclusion: Radiation complications can be vision and eye threatening. Radiation maculopathy is a consequence of higher radiation dose on the macula.
The treatment modalities of radiation maculopathy are rather ineffective.